An urgent need for robotic surgery training, accessible to all surgeons
Strasbourg, February 18th, 2026
Robotic surgery has experienced rapid growth in recent years. Approximately 10,000 robotic surgical systems are currently installed in hospitals worldwide¹.
In France, as in many other countries, this discipline is gradually becoming established in operating rooms, driven by its recognized clinical benefits: enhanced precision, minimally invasive procedures, improved surgical comfort, and faster patient recovery. Yet behind this technological momentum, a major issue remains: ensuring access to appropriate, standardized, and generic training for all surgeons.
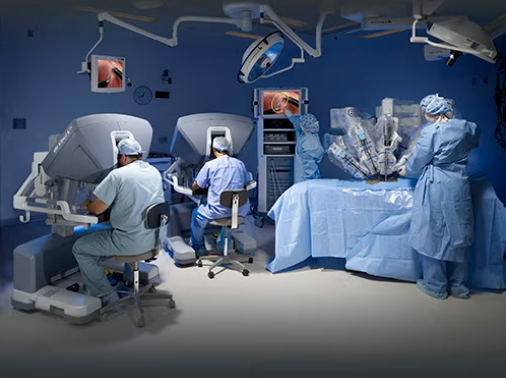
Da Vinci robot
Source: Elsan.com
In France, technological adoption is outpacing training
In France, the current limitations of robotic surgery training have been clearly highlighted by the Académie Nationale de Médecine. While the number of surgical robots installed across the country continues to rise – with more than 300 robots deployed in public and private healthcare institutions in 2025² – access to structured training remains uneven depending on institutions, regions, and specialties.
Training still largely relies on industry-dependent programs, mentorship models, or progressive learning directly in the operating room. This situation creates several challenges: unequal access, lack of standardized competencies, and increased pressure on both surgical teams and patients.
As emphasized by the Académie Nationale de Médecine, the expansion of robotics must be accompanied by standardized university curricula and recognized certification examinations to ensure high-quality initial and continuing education for surgical teams².
In emerging countries: rapid deployment of robotics… without a training ecosystem
Beyond Europe, the issue is even more pronounced in emerging countries, where robotic surgery is beginning to expand rapidly. A recent study conducted in China³ (an emerging country in the adoption of robotic surgery) highlights that, despite the rapid increase in robotic procedures, by the end of 2022 there were only two dedicated robotic surgery training centers nationwide, alongside a clear shortage of formal training programs and surgeons benefiting from structured education.
This rapid deployment faces a significant challenge: the training ecosystem is not always ready. Expert centers are rare, trained instructors are few, and mentorship opportunities are limited. In this context, reliance on occasional training sessions – often costly and difficult to replicate – slows down the effective adoption of the technology.
Democratizing training therefore becomes an issue of healthcare sovereignty: without accessible, standardized, and locally deployable solutions, robotic surgery risks remaining confined to an elite group of institutions, to the detriment of equitable access to care.
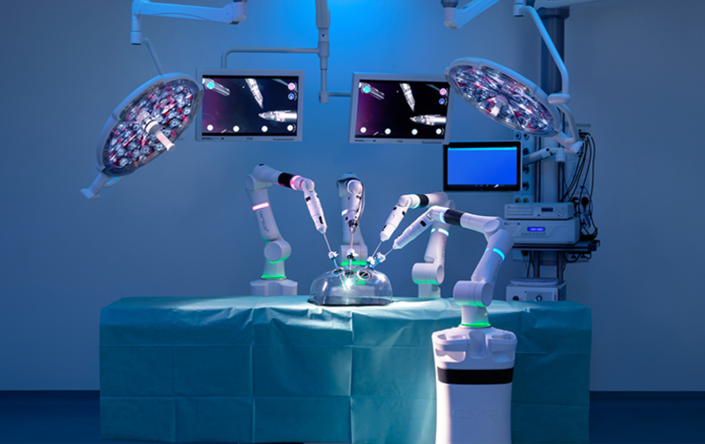
Surgery robot VERSIUS from CMR Surgical
Source: Ircad France
Robotic surgery: toward a more diversified industrial landscape
The robotic surgery market is now opening up to numerous new players, offering platforms with varied architectures, interfaces, and uses. New companies are emerging, and the use of robotics in surgery is expanding into orthopedics, endovascular procedures, neurosurgery, and beyond².
This diversification represents a major opportunity, but it also creates an unprecedented training challenge. Unlike a period dominated by a single industry player, it is now difficult – and undesirable – for training to be driven exclusively by manufacturers. As highlighted by the Académie Nationale de Chirurgie⁴, robotic surgery is entering a phase of maturity in which generic, independent, and standardized training has become essential, similar to what occurred in laparoscopic surgery.
This does not, of course, exclude the legitimate need for system-specific training. However, such programs should complement – not replace – a common foundation of robotic competencies: ergonomics, hand–eye coordination, instrument management, safety, decision-making, and anticipation of complications.

